Eyelid skin is thin and susceptible to sun damage therefore eyelids are commonly affected by skin cancers like basal cell carcinoma, squamous cell carcinoma, and rarely melanomas. Dr. Kopelman has extensive experience restoring the appearance and function of patients who have had skin tumors removed. Eyelid lacerations can occur from accidents and dog bites resulting in torn eyelid margins. These lacerations disrupt the margins of the eyelids which produce misalignment of the eyelashes and margin which may produce cosmetic deformities as well as constant irritation and tearing. Therefore, it is imperative that an oculoplastic surgeon, like Dr. Kopelman, restore the natural contours of the eyelids as well as repair the lacerated tear ducts in order to prevent chronic tearing and infections. Other forms of trauma may also include broken facial bones or orbital fractures that may occur from a blow to the midface. Patients with fractures commonly report that they accidentally fell and hit their face, got injured in a fight, or a barbell accidentally fell and hit them in the face while at the gym. Dr. Kopelman has 30 plus years experience resetting broken facial bones.


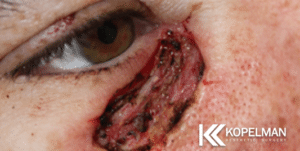
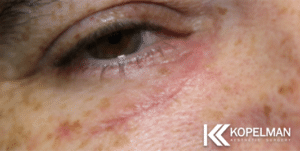
These Eyelid Reconstructive before and after pictures represent actual patients from Dr. Kopelman. They will help you to set realistic goals for your own surgical outcome. Click on a patient to learn more about their reconstructive eyelid surgery.
“Dr. Kopelman every day I look at my daughter’s beautiful eye and thank God for you and your skills. I am so grateful that you were there for us at such a tragic time. Because of you, our daughter is whole again. I didn’t dare hope that with a dog bite so severe, our daughter’s eye could look normal again. It does! The tear duct functions well! I appreciate how kind and caring you have been. Thank you and God Bless.
~ Parent's of a young child injured from dog bit to the eye ~
There are many challenges involved in restoring normal form and function to the eyelids and orbit therefore you should turn to a world class expert like Dr. Kopelman. As an oculoplastic surgeon, Dr. Kopelman has thirty-five years performing reconstructive eyelid surgery following any eyelid traumas including repairing eyelid tumors, lacerations or orbital blowout fractures.
Reconstructive Surgery indicated for
Dr. Kopelman has the experience that counts when you want superb results to restore your eyelid contours.
Schedule a Consultation
For Reconstructive Eyelid Surgery
To schedule a private consultation with Dr. Kopelman,
please call the office or request an appointment online.
Follow me around the web
Dr. Joel Kopelman is a Facial Oculoplastic Surgeon in New York City and New Jersey Performing Eyelid Surgery, Browlifts and Facelifts

Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.